Osteoarthritis of the Spine
A degenerative joint condition affecting the spinal discs and joints
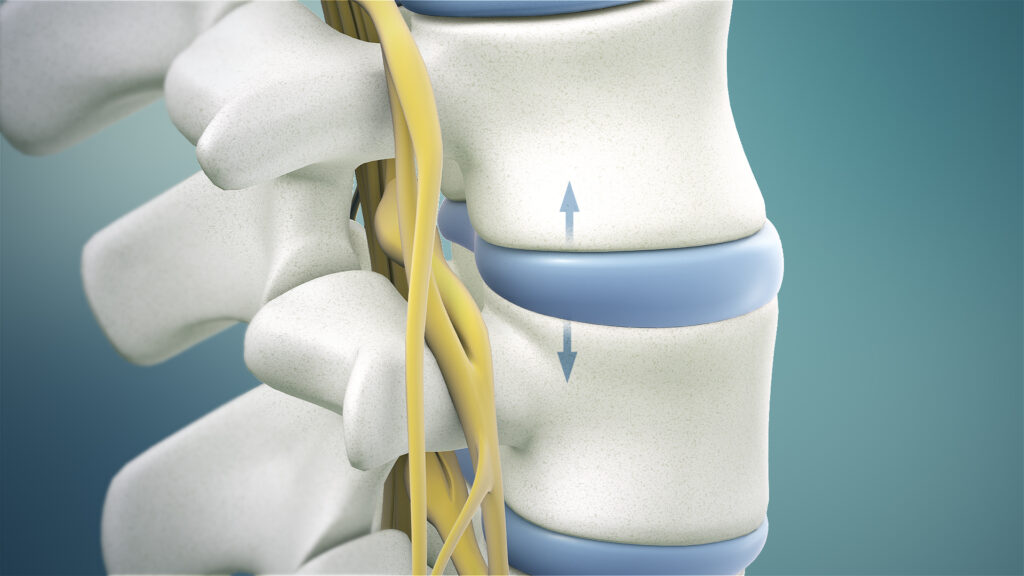
Osteoarthritis of the spine, sometimes called spinal osteoarthritis, is a degenerative joint condition where the protective cartilage in the spinal joints gradually breaks down. It most commonly affects the neck (cervical spine) and lower back (lumbar spine).
As the cartilage wears away, the bones can rub against each other, leading to pain, stiffness, reduced mobility, and sometimes inflammation. In some cases, bone spurs (osteophytes) may also develop, which can further contribute to discomfort or nerve irritation.
The severity of symptoms varies from person to person. While some experience only mild stiffness, others may develop more persistent pain that affects daily activities. Management options range from lifestyle changes and physiotherapy to medications or, in more advanced cases, surgical treatment.
Causes of Osteoarthritis of the Spine
Several factors can contribute to the development of osteoarthritis in the spine, including:
- Age: The risk of developing osteoarthritis increases with age as the cartilage naturally wears down over time.
- Genetics: A family history of osteoarthritis can increase the likelihood of developing the condition.
- Previous Injuries: Past injuries to the spine, such as fractures or sprains, can predispose individuals to osteoarthritis.
- Repetitive Stress: Occupations or activities that involve repetitive movements or heavy lifting can lead to wear and tear on the spinal joints.
- Obesity: Excess body weight places additional stress on the spine, contributing to the degeneration of cartilage.
Symptoms of Osteoarthritis of the Spine
The symptoms of spinal osteoarthritis can vary in intensity and may include:
- Back Pain: A persistent, dull ache in the back that may worsen with activity or prolonged sitting.
- Stiffness: Stiffness in the spine, particularly in the morning or after prolonged periods of inactivity.
- Reduced Range of Motion: Difficulty bending, twisting, or performing certain movements due to stiffness and pain.
- Nerve Symptoms: In some cases, osteoarthritis can lead to nerve compression, causing symptoms such as tingling, numbness, or weakness in the legs or arms.
Diagnosis of Osteoarthritis of the Spine
Diagnosis usually begins with a medical history and physical examination. Your doctor will ask about symptoms such as back or neck pain, stiffness, or reduced mobility, and how these affect your daily activities. They may also check posture, range of motion, and neurological function to identify any signs of nerve involvement.
Physical examination
- Assessment of spinal movement and flexibility.
- Observation for tenderness or changes in alignment.
- Neurological checks, including reflexes, strength, and sensation, if nerve irritation is suspected.
Imaging tests
To confirm the diagnosis and assess the extent of joint changes, imaging may be recommended:
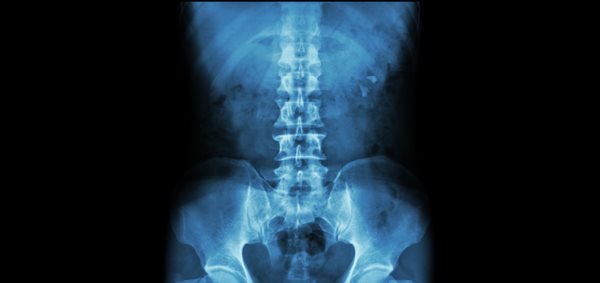
- X-rays – Can show narrowing of the disc spaces, bone spurs, and other degenerative changes.
- Magnetic resonance imaging (MRI) – Provides detailed images of discs, joints, and nerves, and can detect inflammation or nerve compression.
- Computed tomography (CT) scan – May be used for more detailed bone assessment if needed.
These tests, combined with the clinical examination, help determine whether symptoms are due to osteoarthritis or another spinal condition, and guide the most appropriate treatment plan.
Treatment Options for Osteoarthritis of the Spine
Management of spinal osteoarthritis focuses on relieving pain, improving mobility, and supporting spinal health. The choice of treatment depends on the severity of symptoms, the specific part of the spine affected, and the individual’s overall health and activity level.
Non-surgical treatments
Most people find improvement through non-surgical approaches, which may include:
- Physiotherapy – Targeted exercises to strengthen supporting muscles, improve flexibility, and maintain posture.
- Medications – Non-steroidal anti-inflammatory drugs (NSAIDs), analgesics, or muscle relaxants may be used to help reduce pain and stiffness.
- Injections – Corticosteroid or facet joint injections may provide temporary relief from inflammation and discomfort.
- Lifestyle modifications – Weight management, regular low-impact exercise (such as walking or swimming), and ergonomic adjustments to daily activities can help reduce strain on the spine.
- Heat or cold therapy – Applying heat or ice packs may ease stiffness and pain.
Surgical treatments
Surgery is considered only when conservative measures do not provide sufficient relief, or when osteoarthritis causes significant nerve compression or instability. Options may include:
- Spinal decompression – Removal of bone or tissue pressing on nerves to reduce pain and neurological symptoms.
- Spinal fusion – Joining two or more vertebrae to stabilise the spine in cases of severe degeneration.
The decision to proceed with surgery is made on an individual basis, taking into account the extent of spinal changes, symptoms, and the patient’s overall health and goals.